At Mark Hinds Optometrists we try our best to be involved in pre-release products and research. As Dr Hinds’ shifts into Ophthalmic clinical Trials, we have the opportunity to have our patients be the foundation of the future of eye care. Through this we trial treatments, drops and devices from pharmaceutical or biotech companies from around the world who are looking to release their innovative treatments on the market.
One of our optometrists may ask if you have any interest in participating. If you have a ocular condition and may be interested, please click here: Ophthalmic Trials Australia.
For those of you with Dry Eye Disease, you may have noticed in our dry eye suite we have 2 new treatments, Zest (Zocular eyelid system technology) and Rinsada.
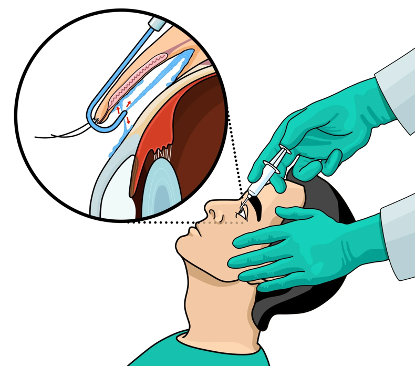
Rinsada is an irrigating lid retractor, under the same premise of a sinus flush, Rinsada pushes 7mls of Saline under your top lid and 3mls under your bottom lid. This is supposed to deliver irrigation to the conjunctiva and bulbar conjunctiva simultaneously. Rinsada uses high flow irrigation to remove ocular surface irritants and inflammation. Despite looking rather scary it is surprisingly a pleasant feeling when being “Rinsada’d”. After doing this you are still to remain taking your normal eye drops, this is a treatment which is used in tandem with your current treatments to improve or extend relief. If you want to know more, please click here: Rinsada.
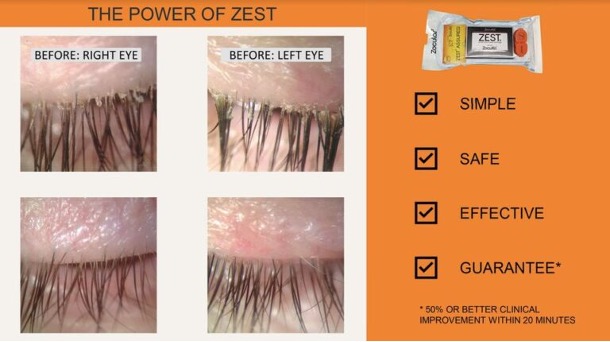
Zest is a deep cleansing of the lids to revitalise your eyes for lasting comfort. Aimed to refresh the ocular surface and clear the eyelids/lashes. The procedure is to use a cotton swab to rub in the zest gel onto the eye lids (eyes closed), this will be done with a fast (and soft) motion to make the gel begin to foam.
At this point in the procedure, if stinging occurs this is most likely due to makeup (or equivalent) between the gel and your skin. If this occurs, please let the optometrist know so they can stop the procedure and allow for you to either come back another day with no make-up on or for you to clean it off.
The optometrist will continue to rub the zest until it begins to foam, at that point the foam will be wiped off your eye. You will then be asked to open your eye, the optometrist will then squirt a second zest product (Saline) approximately 4-5 times into your lower lid, wiping away any excess fluids in the process.
This procedure will then be repeated with the other eye.