“THIS IS WHAT WE DO” – Mark Hinds Optometrist
Rigid Gas Permeable Contact Lenses (RGP) are made from plastic polymers that allow the flow of oxygen to the eye. RGP’s are also easier to clean than soft contact lenses and better deposit resistant Anyone who knows anything about contact lenses will have detailed knowledge of RGP’s.
Mark Hinds Optometrists is one of Australia’s leading practices in specialty contact lens work. Patients are often referred eery week from corneal specialists, optometrists and tertiary eye hospitals for complex and challenging fitting. We have extensive fitting sets, a RGP contact lens polishing unit on site, RGP contact lens solutions (sold in clinic) and a corneal topographer with computer based RGP contact lens fitting simulations and Zeiss OCT with anterior segment capability to establish exact corneal fit. Dr Hinds has been teaching how to fit these lenses at QUT’s school of optometry since 2004 and has hundreds (if not thousands) of patients successfully wearing them. Dr Hinds lectures on this topic both at the national and international level with his expertise being sought by leading contact lens manufacturers and biotech/pharmaceutical companies, in the world of clinical trials, for advice.
RGP’s are especially beneficial for patients with/or are:
- Astigmatism
- Post-graft
- Post laser
- Post PRK
- Post PK
- Traumatised Corneas (etc.)
Many of our patients have very poor vision (even in spectacles) often have the ability to obtain 20/20 vision with well-designed RGP contact lenses.
New technologies in hybrid contact lenses are now available in the form of Duette High Definition, Duette Multifocal and the successor to the ClearKone hybrid contact lens, the Duette UltraHealth and the new FC range for post refractive surgery ectasia.
For scleral and mini-scleral contact lenses in Australia we are one of the busiest fitters in the country. We fit patients with vast corneal diseases including (but not limited to):
- Keratoconus
- Pellucid marginal degeneration
- Terrien’s marginal degeneration
- Corneal grafts
- Ocular surface disease
- Extreme dry eye
- Corneal hyperalgesia
- Corneal irregularity
- Ocular disfigurement
Please see the videos below for any more information.
Cleaning your Scleral, Mini-Scleral, Corneo-Scleral and RGP Contact Lenses with BOSTON solutions.
Cleaning your Scleral, Mini-Scleral, Corneo-Scleral and RGP Contact Lenses with MENICARE solution.
Cleaning your Scleral, Mini-Scleral, Corneo-Scleral and RGP Contact Lenses with PEROXIDE solutions.
Cleaning your Scleral, Mini-Scleral, Corneo-Scleral and RGP Contact Lenses with BIOTRUE solution.
Keratoconus
Keratoconus is a progressive disease, often appearing in the teens or early twenties, in which the cornea thins and changes shape. The cornea is normally a round or spherical shape, but with keratoconus the cornea bulges, distorts and assumes more of a cone shape. This affects the way light enters the eye and hits the light-sensitive retina, causing distorted vision. Keratoconus can occur in one or both eyes.
Keratoconus Symptoms and Signs
Keratoconus can be difficult to detect, because it comes on slowly. You may have distorted and blurred vision. You might also notice glare and light sensitivity. Keratoconic patients often have prescription changes each time they visit their optometrist. It’s not unusual to have a delayed diagnosis of keratoconus, if the practitioner is not familiar with the early-stage symptoms of the disease.
What Causes Keratoconus?
Causes of keratoconus are unclear. A genetic link may exist, as you may find several keratoconics within an extended family.
Keratoconus Treatment
In the mildest form of keratoconus, spectacles or soft contact lenses may help. But as the disease progresses and the cornea thins and changes shape even more, spectacles or soft contacts will no longer correct your vision. Rigid gas permeable contact lenses are the next correction method of choice.
The firmer material of a rigid contact lens holds the cornea in place better than a soft contact lens. Fitting contact lenses on a keratoconic cornea is delicate and time-consuming. You can expect frequent return visits to fine-tune the fit and the prescription. The process will begin again when the cornea thins and distorts even more, altering the contact lens fit and prescription needed for clear, comfortable vision.
Keratoconus – the statistics:
- 80% of patients present before the age of 40 years.
- Keratoconus is bilateral in 80% patients and unilateral in 20% patients.
- Family history of keratoconus occurs in 15% of patients.
- A history of atopy and eye rubbing is obtained in 45% and 10% patients.
- Treatment modalities at follow-up included rigid gas-permeable contact lenses (CL) 50%.
- Corneal graft 25%.
- No treatment 13%.
- Spectacles 9%.
- Soft CL (2%).
- Riboflavin treatment / corneal cross linking (numbers still growing).
- The annual corneal graft rate is about 3% per year per eye.
- With careful contact lens fitting most keratoconus patients will not require a corneal graft.
KERATOCONUS TOPOGRAPHICAL MAP CENTRAL CONE
Corneal Specialists / Ophthalmologists

Many of our patients who see us for specialty contact lens fitting have various degrees of corneal ectasia / conditions and ocular surface dysfunction. Hence we are fortunate to co-manage with some of the world’ best corneal surgeons including
- Dr Andrew Apel Dr Andrew Apel
- Dr Peter Beckingsale Dr Peter Beckingsale
- Dr Brendan Cronin Queensland Eye Institute /
- Dr James McAlister www.eyesmatter.com.au
- Dr Luke Maccheron Brisbane North Eye Centre
- Dr Hamish McKee Dr Hamish McKee – Laser Sight Centre Sunshine Coast QLD
We do watch for potential corneal cross linking (CXL) patients as it is indicated for progressive keratoconus. Outcomes with this procedure are promising when patient selection is good. Numbers at this stage indicate >90% success rate with success being judged on corneal stabilizaton. We are noticing a small but measurable improvement in visual acuity – but it must be noted that this procedure is not a refractive corrective surgery but rather a prevention of further progression and the 3 & 5 year data does look good (see reference below). Some patients (about 3-4%) do get some significant corneal haze and may experience some decrease in vision post operatively. The numbers here are growing and we have several hundred patients with great outcomes post CXL.
Key criteria at this stage appear to be:
- Documented progression (>1DC per year)
- Pachimetry > 450um
- Corneal steepness < 58D (with repeated measures of corneal topography without contact lenses in for several days)
- Generally < 35 years of age
- Good visual acuity
(Wollensak G. Crosslinking treatment of progressive keratoconus: New Hope. Current Opinion in Opthalmology 2006; 17: 356-360)
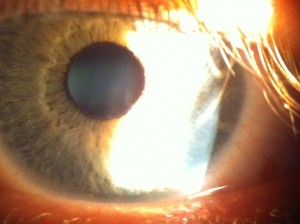
Advanced keratoconus 18 months post riboflavin / corneal crosslinking
Astigmatism
Astigmatism is the most common vision problem, however most people don’t know what it is. It may accompany nearsightedness or farsightedness. Usually it is caused by an irregularly shaped cornea (called corneal astigmatism). But sometimes it is the result of an irregularly shaped lens, which is located behind the cornea; this is called lenticular astigmatism. Either kind of astigmatism can usually be corrected with spectacles or contact lenses.
Astigmatism symptoms and signs
If you have only a small amount of astigmatism, you may not notice it or have just slightly blurred vision. But sometimes uncorrected astigmatism can give you headaches or eyestrain, and distort or blur your vision at all distances. It’s not only adults who can be astigmatic. Dr. Karla Zadnik, an optometrist at Ohio State University School of Optometry, found in a recent study of 2,523 children that more than 28% of them had astigmatism.
Children may be even more unaware of the condition than adults, and they are unlikely to complain of the blurred or distorted vision. Unfortunately, astigmatism can affect their ability to see well in school and during sports, so it’s important to have their eyes examined at regular intervals in order to detect any astigmatism early on.
What causes astigmatism?
Astigmatism occurs when the cornea is shaped more like an Australian Rules football than a spherical tennis ball, which is the normal shape. In most astigmatic eyes, the oblong or oval shape causes light rays to focus on two points in the back of your eye, rather than on just one. This is because, like an Australian rules football, an astigmatic cornea has a steeper curve and a flatter one.
In regular astigmatism, the meridians in which the two different curves lie are located 180 degrees apart. In irregular astigmatism, the two meridians may be located at something other than 180 degrees apart; or there are more than two meridians.
Regular astigmatism is usually easy to correct (see treatments below), but irregular astigmatism can be complicated and more difficult to correct, depending on the extent of the irregularity and its cause.
Usually astigmatism is hereditary: many people are born with an oblong cornea, and the resulting vision problem may get worse over time. But astigmatism may also result from an eye injury that has caused scarring on the cornea, from certain types of eye surgery, or from keratoconus, a disease that causes a gradual thinning of the cornea.
Astigmatism treatment
Unless it is extreme, astigmatism can be compensated for satisfactorily with spectacles or contact lenses. If your spectacles or contact lens prescription contains three parts rather than one, your eyecare practitioner has found some astigmatism in one or both of your eyes.
Many people with astigmatism believe that they can’t wear contact lenses, or that only rigid gas permeable contact lenses can correct astigmatism. This was true many years ago, but now there are soft contacts that correct astigmatism; they are called toric contact lenses.
Toric lenses have a special correction built into them and may also contain a prescription for nearsightedness or farsightedness if you need it. While soft torics work well for many people, if you have severe astigmatism, you’ll likely do better with Rigid Gas Permeable contact lenses or spectacles. Our specialist contact lense optometrists can advise you.
Corneal Topography
We have invested in the most up to date and accurate corneal mapping equipment with integrated contact lens designing software to help us fit the most challenging eyes with contact lenses.
Corneal topography is interpreted much like other topography maps. The cool shades of blue and green represent flatter areas of the cornea, while the warmer shades of orange and red and represent steeper areas. This corneal map allows the us to formulate a “3-D” perspective of the cornea’s shape. Measuring the ocular surface is important for fitting contact lenses, and calculating lens power.
Corneal topography is a process for mapping the surface curvature of the cornea, similar to making a contour map of land. The cornea is a clear membrane that covers the front of the eye and is responsible for about 70 percent of the eye’s focusing power. To a large extent, the shape of the cornea determines the visual ability of an otherwise healthy eye but if the cornea is too flat, too steep, or unevenly curved, less than optimum vision results can occur.
The purpose of corneal topography is to produce a detailed description of the shape and power of the cornea. At Mark Hinds Optometrists we use computerized imaging technology, and the 3-dimensional map produced by the corneal topographer aids us in the diagnosis, monitoring, and treatment of various visual conditions. Riboflavin or corneal crosslinking treatment for keratoconus and pellucid marginal degeneration requires evidence of progression and this is one of the main tools we use for that purpose. Our corneal topography system is state of the art and is often aided by our OCT (Optical Coherence Tomographer) for fitting very challenging corneas with rigid gas permeable and often mini-scleral or scleral contact lenses. This device is also critical to fitting orthoK contact lenses as you simply can not fit orthokeratology or corneal reshaping (CRT) contact lenses without it.
For our downloadable PDF’s, click the link below: